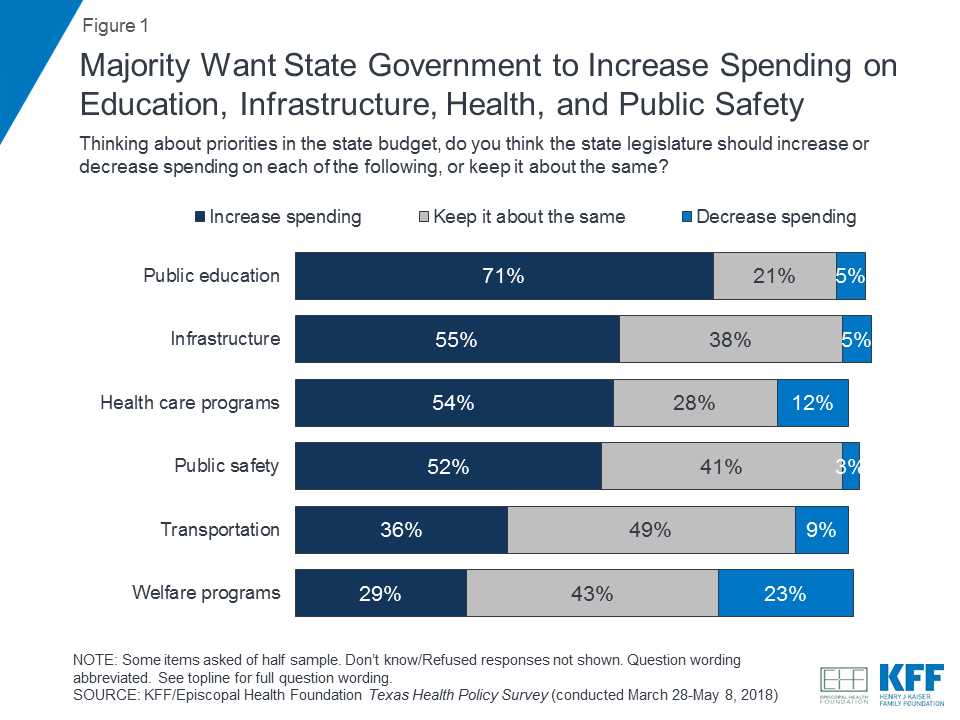
Texas is renowned for its size and diversity, but when it comes to healthcare, does the Lone Star State measure up? This article explores the question of whether Texas possesses a commendable healthcare system. By examining key factors such as accessibility, quality, and affordability, we aim to provide a thorough analysis that sheds light on the strengths and weaknesses of healthcare in the region. So, grab your stethoscope and join us as we dissect the intricacies of Texas’ healthcare landscape.

This image is property of stateofreform.com.
Access to Healthcare
Healthcare Coverage
Access to healthcare coverage is a critical aspect of ensuring that individuals can receive the medical care they need. In Texas, there are multiple options available for healthcare coverage. The most common forms of coverage include private insurance, marketplace plans, Medicaid, and being uninsured. Private insurance is typically obtained through employers or purchased directly from insurance companies. Marketplace plans, on the other hand, are offered through the Health Insurance Marketplace, where individuals can compare and purchase health insurance plans. Medicaid provides coverage to low-income individuals and families, and eligibility is determined based on income and other factors. Unfortunately, Texas has not expanded Medicaid, which has left many low-income individuals without access to affordable healthcare coverage. Lastly, a significant number of Texas residents remain uninsured, posing challenges to accessing healthcare services.
Insurance Rates
When considering the quality of a healthcare system, it is essential to evaluate insurance rates. Insurance rates in Texas have been a cause for concern, as they have historically been higher compared to the national average. This can be attributed to several factors, including the high cost of healthcare services, the number of uninsured individuals, and the overall health status of the population. Without adequate insurance coverage, individuals may face significant financial burden when seeking medical care. It is crucial for policymakers and stakeholders to address insurance rates to ensure that healthcare remains affordable and accessible for all Texans.
Medical Facilities
The availability and quality of medical facilities play a vital role in determining the overall healthcare system’s effectiveness. In Texas, there are numerous medical facilities, ranging from small clinics to large hospitals and specialized healthcare centers. Urban areas often have a greater concentration of medical facilities, which increases access to healthcare services. However, rural areas face challenges in terms of access to medical facilities. The shortage of healthcare providers and limited healthcare infrastructure in rural areas can result in individuals having to travel long distances to receive necessary care. Improving the distribution of medical facilities across the state, particularly in underserved areas, is essential to ensure that all Texans have equal access to healthcare services.
Rural Healthcare
Rural healthcare in Texas presents unique challenges compared to urban areas. The limited availability of medical facilities, healthcare professionals, and specialized services can significantly impact individuals living in rural areas. The shortage of healthcare providers, including physicians, nurses, and specialists, in these areas often leads to longer wait times for appointments and reduced access to specialized care. Additionally, limited transportation options and long travel distances can further impede rural residents’ ability to access healthcare. It is crucial for policymakers to address these disparities and implement strategies to improve access to healthcare in rural areas, such as telehealth initiatives and incentives for healthcare professionals to practice in underserved regions.
Quality of Healthcare
Healthcare Professionals
The quality of healthcare in Texas relies heavily on the proficiency and expertise of healthcare professionals. Texas boasts a large number of healthcare professionals, including physicians, nurses, and other allied health professionals. However, disparities in the distribution of healthcare professionals across the state can affect access to quality care. Urban areas tend to have a higher concentration of healthcare professionals, while rural areas often struggle with shortages. Addressing these disparities and ensuring a sufficient healthcare workforce across all regions is crucial to maintaining high-quality healthcare in Texas.
Cancer Care
Cancer care is a critical aspect of healthcare quality, as it affects a significant number of individuals and requires specialized treatment. In Texas, access to cancer care can vary depending on geographical location and healthcare infrastructure. Urban areas often have comprehensive cancer centers offering advanced treatments, clinical trials, and multidisciplinary teams of healthcare professionals. However, individuals in rural areas may face challenges in accessing these specialized cancer care facilities, leading to delays in diagnosis and treatment. Efforts to improve cancer care in Texas should focus on expanding access to specialized cancer centers, promoting screening and early detection programs, and ensuring comprehensive care for all Texans regardless of their geographical location.
Patient Safety
Ensuring patient safety is a fundamental component of providing high-quality healthcare. In Texas, various initiatives and regulations are in place to promote patient safety. Healthcare facilities are required to comply with strict guidelines and protocols to minimize medical errors, prevent hospital-acquired infections, and improve overall patient outcomes. Additionally, regulatory bodies and professional organizations continue to establish quality and safety standards to guide healthcare providers in delivering safe and effective care. Monitoring and evaluating patient safety measures are essential to identifying areas for improvement and maintaining high-quality healthcare across the state.
Maternal and Child Health
The quality of healthcare in Texas extends to maternal and child health, as the well-being of mothers and children is crucial for a thriving population. Maternal and child health outcomes in Texas have been a point of concern, as the state has experienced higher rates of maternal mortality and infant mortality compared to the national average. Efforts to improve maternal and child health should focus on enhancing prenatal care, reducing barriers to healthcare access for pregnant women, promoting breastfeeding, and ensuring comprehensive healthcare services for children. Collaborative initiatives between healthcare providers, public health agencies, and community organizations can contribute to improved maternal and child health outcomes in Texas.
Healthcare Rankings
Evaluating healthcare rankings and benchmarks can provide insights into the overall quality and performance of a healthcare system. Texas has faced challenges in healthcare rankings, often falling behind other states in various aspects of healthcare delivery. These rankings consider factors such as access to care, healthcare outcomes, patient satisfaction, and public health measures. While Texas has made efforts to address these areas of concern, there is still room for improvement. Regular assessment of healthcare rankings can help policymakers and stakeholders identify areas for targeted intervention and implement strategies to enhance the quality of healthcare in Texas.

This image is property of www.kff.org.
Healthcare Affordability
Healthcare Costs
Healthcare costs play a significant role in determining the affordability of healthcare for individuals and families. In Texas, healthcare costs have been a point of concern, as they tend to be higher compared to the national average. Factors contributing to higher healthcare costs include the high cost of medical procedures and treatments, prescription drug prices, and the overall health status of the population. Addressing healthcare costs is crucial to ensuring that healthcare remains affordable and accessible for all Texans.
Citizens’ Financial Burden
High healthcare costs can result in significant financial burdens for individuals and families. Medical expenses, including premiums, deductibles, copayments, and out-of-pocket costs, can contribute to financial hardship, particularly for those with limited financial resources. To mitigate these burdens, programs like Medicaid and marketplace subsidies aim to provide financial assistance to eligible individuals and families. However, broader initiatives to address healthcare costs and improve affordability are necessary to ensure that Texans are not burdened with excessive healthcare expenses.
Affordability for the Uninsured
For individuals without health insurance coverage, healthcare affordability can be especially challenging. Without insurance, individuals often face higher out-of-pocket costs, limited access to discounted rates negotiated by insurance providers, and less financial protection against medical expenses. Although safety net programs and community clinics exist to provide care to the uninsured, ensuring affordable healthcare for this population remains a significant challenge. Expanding access to insurance coverage and implementing cost containment measures can help improve healthcare affordability for the uninsured in Texas.
Prescription Drug Costs
The rising cost of prescription drugs has been a matter of concern for individuals, healthcare providers, and policymakers alike. In Texas, the affordability of prescription drugs poses challenges, particularly for individuals with chronic conditions who rely on ongoing medication therapy. High prescription drug costs can result in individuals foregoing necessary medications or facing financial strain. Exploring options such as price transparency, generic drug utilization, and prescription drug assistance programs can contribute to reducing prescription drug costs and enhancing healthcare affordability for Texans.
Health Outcomes
Life Expectancy
Life expectancy is a crucial health outcome indicator that reflects the overall health and well-being of a population. In Texas, life expectancy has been slightly lower compared to the national average. Several factors contribute to this, including health behaviors, socioeconomic factors, access to healthcare, and the prevalence of chronic diseases. Addressing disparities in life expectancy requires a multifaceted approach that involves promoting healthy lifestyles, improving access to preventive care and chronic disease management, and addressing social determinants of health.
Mortality Rates
Mortality rates provide insights into the overall health outcomes of a population. In Texas, mortality rates have been influenced by various factors, including access to healthcare, chronic diseases, and public health initiatives. Higher mortality rates for certain conditions, such as heart disease, stroke, and cancer, highlight the need for targeted interventions and improved access to high-quality care. Collaborative efforts between healthcare providers, public health agencies, and community organizations are crucial to reducing mortality rates and improving overall health outcomes for Texans.
Preventive Care
Preventive care plays a pivotal role in promoting health and well-being, preventing the onset of diseases, and detecting conditions at an early stage when they are more treatable. In Texas, access to preventive care varies across populations and geographic locations. Efforts to improve preventive care should focus on increasing awareness of recommended screenings and vaccinations, ensuring access to preventive services through insurance coverage, and promoting healthcare provider engagement in delivering evidence-based preventive care to their patients. A robust preventive care framework contributes to better health outcomes and overall population health in Texas.
Chronic Disease Management
Chronic diseases, such as diabetes, heart disease, and respiratory conditions, pose a significant burden on individuals and the healthcare system alike. In Texas, the prevalence of chronic diseases is relatively high compared to other states. Effective chronic disease management requires a comprehensive approach that includes access to affordable healthcare, patient education, lifestyle modifications, and ongoing monitoring and support. Collaborative efforts between healthcare providers, community organizations, and patients are essential to managing chronic diseases effectively and improving health outcomes for individuals with chronic conditions in Texas.

This image is property of www.kff.org.
Health Disparities
Racial and Ethnic Disparities
Health disparities based on race and ethnicity continue to persist in Texas. Certain racial and ethnic populations face greater challenges in accessing high-quality healthcare and experience higher rates of chronic diseases and adverse health outcomes. Addressing racial and ethnic disparities requires a multifaceted approach that involves improving access to care, culturally competent healthcare delivery, and addressing social determinants of health to reduce systematic barriers that contribute to these disparities. Efforts to promote health equity, enhance diversity in the healthcare workforce, and engage communities in healthcare decision-making are crucial to reducing racial and ethnic disparities in Texas.
Income-Based Disparities
Income-based disparities in healthcare access and outcomes are another significant concern in Texas. Low-income individuals often face barriers to accessing healthcare due to limited insurance coverage, financial constraints, and other socioeconomic factors. Efforts to address income-based disparities should focus on expanding access to affordable insurance coverage, enhancing safety net programs, promoting healthcare workforce diversity in underserved areas, and addressing social determinants of health that contribute to these disparities. Comprehensive initiatives that ensure healthcare access and improve health outcomes for all socioeconomic groups are essential to reducing income-based disparities in Texas.
Rural vs. Urban Disparities
Disparities between rural and urban areas in terms of healthcare access and outcomes have been a persistent challenge in Texas. Rural areas often face shortages of healthcare professionals and limited healthcare infrastructure, resulting in reduced access to care and poorer health outcomes. Efforts to address rural-urban disparities should focus on improving healthcare infrastructure in underserved areas, expanding access to telehealth services, providing financial incentives for healthcare professionals to practice in rural regions, and implementing targeted public health initiatives. Bridging the gap between rural and urban healthcare can contribute to reducing disparities and improving overall health in Texas.
Access Disparities
Access disparities refer to differences in the ability of individuals to obtain timely and appropriate healthcare services. In Texas, access disparities exist across various populations, including those based on race, ethnicity, socioeconomic status, and geographical location. To address access disparities, policymakers and stakeholders must focus on improving healthcare infrastructure, addressing workforce shortages, implementing telehealth initiatives in underserved areas, and ensuring culturally competent care for diverse populations. Timely and equal access to high-quality healthcare is crucial to reducing access disparities and promoting health equity in Texas.
Healthcare Infrastructure
Hospital Beds
Hospital beds are a critical component of a healthcare system’s infrastructure as they provide acute and specialized care for patients. In Texas, the number of hospital beds varies across geographic regions, with urban areas often having higher bed capacities compared to rural areas. Ensuring an adequate number of hospital beds is crucial to meeting the healthcare needs of the population, especially during public health emergencies or natural disasters. The distribution of hospital beds should be evaluated regularly to identify areas with potential shortages and implement strategies to address these gaps in Texas.
Physician-to-Population Ratio
The availability of physicians is a key factor in determining the accessibility and quality of healthcare. In Texas, there is significant variation in the physician-to-population ratio across different regions. Urban areas tend to have a higher concentration of physicians, while rural and underserved areas often face shortages. To address this disparity, efforts should focus on promoting the recruitment and retention of healthcare professionals in underserved regions, implementing loan forgiveness programs, and expanding residency and training opportunities for physicians. Ensuring a sufficient physician supply across all regions is essential to improving healthcare infrastructure and access to care in Texas.
Technology Integration
Technology integration in healthcare has the potential to improve efficiency, enhance patient outcomes, and expand access to care. In Texas, the adoption and integration of technology in healthcare have been increasing, with telehealth being a prominent example. Telehealth allows patients to access healthcare services remotely, improving access in underserved areas and reducing barriers to care. Additionally, electronic health records (EHRs) have become prevalent, allowing for better coordination of care, patient data sharing, and improved patient safety. Continued investment in technology integration, including broadband access, telehealth infrastructure, and EHR implementation, can contribute to an enhanced healthcare infrastructure in Texas.
Emergency Preparedness
Being equipped to respond to public health emergencies and natural disasters is crucial for a healthcare system’s resilience. In Texas, the experience of hurricanes, floods, and other natural disasters underscores the importance of emergency preparedness. Healthcare facilities must have robust emergency preparedness plans in place to ensure continuity of care during crises. Collaboration between healthcare providers, emergency management agencies, and public health organizations is essential to effectively respond to emergencies and safeguard the health and well-being of Texans.

This image is property of www.kff.org.
Insurance Market
Private Insurance
Private insurance plays a significant role in healthcare coverage in Texas. Many individuals obtain health insurance through their employers or purchase private insurance plans directly from insurance companies. Private insurance offers various plans with different levels of coverage and premiums. However, affordability and access to private insurance can be a concern for some individuals, particularly those with pre-existing conditions or limited financial resources. Regulatory measures to ensure coverage for pre-existing conditions and promote affordability are crucial to maintaining a robust private insurance market in Texas.
Marketplace Plans
The Health Insurance Marketplace provides a platform for individuals to compare and purchase health insurance plans. In Texas, the Marketplace offers a range of plans that cater to different needs and budgets. Marketplace plans are required to cover essential health benefits, including preventive care, maternity care, and prescription drugs. Subsidies are also available for eligible individuals to help make coverage more affordable. However, the affordability and accessibility of marketplace plans can still pose challenges for certain populations. Ensuring a robust Marketplace with a wide range of options and affordability assistance is essential to meeting the healthcare coverage needs of Texans.
Medicaid Expansion
Medicaid provides coverage to low-income individuals and families, including pregnant women, children, and individuals with disabilities. However, Texas has chosen not to expand Medicaid under the Affordable Care Act (ACA). This decision has left many low-income individuals without access to affordable healthcare coverage. Expanding Medicaid would extend coverage to a significant number of uninsured individuals, promoting access to care and reducing the financial burden on low-income Texans. Consideration of Medicaid expansion and exploring alternative coverage options can contribute to a more inclusive and accessible insurance market in Texas.
Uninsured Rates
The uninsured rate in Texas has historically been higher compared to the national average. Many individuals in Texas face barriers to obtaining insurance coverage, such as limited financial resources, lack of employer-based coverage, and eligibility restrictions. The high uninsured rate has implications for healthcare access, affordability, and overall population health. Expanding access to affordable insurance options, promoting enrollment in safety net programs, and addressing systemic barriers to coverage are crucial to reducing the uninsured rate in Texas and ensuring that all residents have access to necessary healthcare services.
Healthcare Policy
State Regulations
State regulations play a significant role in shaping the healthcare landscape. In Texas, various regulations govern the operation and delivery of healthcare services, including licensing requirements, scope of practice regulations, and healthcare facility standards. Regulatory bodies, such as the Texas Medical Board and Texas Department of State Health Services, oversee the enforcement of these regulations to ensure patient safety and quality of care. Continual evaluation and updating of state regulations is essential to adapt to changing healthcare needs and promote patient-centered care in Texas.
Medical Liability
Medical liability refers to the legal accountability of healthcare providers for the quality of care they deliver. Medical malpractice lawsuits can have a significant impact on healthcare providers’ practice patterns, insurance premiums, and overall healthcare costs. In Texas, medical liability reform has been a topic of discussion and action. Tort reform measures, such as caps on non-economic damages and changes to the legal process, have been implemented to address concerns regarding medical liability and its impact on the healthcare system. Striking a balance between ensuring patient rights and fair compensation while protecting healthcare providers from excessive litigation is crucial to promoting a robust healthcare system in Texas.
Telehealth
Telehealth, or the use of technology to provide healthcare services remotely, has gained prominence in recent years. In Texas, the utilization of telehealth has increased, especially in rural areas where access to healthcare services can be limited. Telehealth allows patients to consult with healthcare providers, receive diagnoses, and access follow-up care without physically visiting healthcare facilities. Expanding access to telehealth services, addressing reimbursement and licensing challenges across state lines, and incorporating telehealth into healthcare delivery models can contribute to improved healthcare access and outcomes in Texas.
Public Health Initiatives
Public health initiatives play a crucial role in promoting population health and preventing diseases. In Texas, numerous public health initiatives are in place to address various health concerns. These initiatives encompass areas such as immunizations, disease surveillance and reporting, health education and promotion, environmental health, and emergency preparedness. Collaborative efforts between public health agencies, healthcare providers, community organizations, and individuals are necessary to support effective public health initiatives. Continued investment in public health infrastructure and addressing the social determinants of health can contribute to improved health outcomes for all Texans.
This image is property of scx2.b-cdn.net.
Healthcare Challenges
Obesity Epidemic
Texas faces significant challenges related to the obesity epidemic. The prevalence of obesity is higher compared to the national average, and obesity is associated with increased risks for chronic diseases, including heart disease, diabetes, and certain types of cancer. Addressing the obesity epidemic requires a comprehensive approach that focuses on promoting healthy lifestyles, improving access to nutritious food, enhancing physical activity opportunities, and addressing systemic factors that contribute to obesity. Collaborative efforts between healthcare providers, schools, workplaces, and the community are crucial to combating the obesity epidemic and improving overall population health in Texas.
Mental Health
The availability and accessibility of mental healthcare services continue to be a challenge in Texas. Many individuals face barriers to receiving timely and appropriate mental health treatment, including limited access to mental health providers, stigma, and a fragmented healthcare system. The consequences of untreated mental health conditions can be profound, leading to decreased quality of life, increased risks for physical health problems, and higher healthcare costs. Increasing access to mental healthcare services, enhancing mental health provider capacity, integrating mental health services into primary care, and promoting mental health awareness and education are crucial to addressing the mental health challenge in Texas.
Aging Population
Texas, like many other states, is experiencing demographic changes characterized by an aging population. The older population has specific healthcare needs, including chronic disease management, long-term care, and preventive services. Meeting the needs of the aging population requires a comprehensive approach that encompasses healthcare, social services, and community support. Strategies such as promoting healthy aging, enhancing access to geriatric care, supporting family caregivers, and expanding long-term care options can contribute to ensuring that older Texans receive the care and support they need to maintain their health and well-being.
Access in Rural Areas
As previously mentioned, access to healthcare in rural areas remains a significant challenge in Texas. Rural areas often face shortages of healthcare providers, limited healthcare infrastructure, and reduced access to specialized care. Addressing healthcare access in rural areas requires innovative solutions, such as telehealth initiatives, mobile clinics, and financial incentives for healthcare professionals to practice in rural regions. Collaboration between healthcare providers, policymakers, and community organizations is crucial to identifying and implementing strategies that improve access to healthcare services and reduce disparities between rural and urban areas in Texas.
Healthcare Innovations
Technology Adoption
Technological advancements and their adoption in healthcare can improve the efficiency and quality of care. Texas has seen increased technology adoption in various areas, including electronic health records, telehealth, and remote patient monitoring. Electronic health records streamline information sharing and enhance care coordination, while telehealth and remote patient monitoring improve access to care and enable remote monitoring of patients’ health status. Continued investment in technology adoption, ensuring interoperability between systems, and supporting healthcare providers in embracing new technologies can contribute to improved healthcare delivery and outcomes in Texas.
Value-Based Care
Value-based care models emphasize delivering high-quality care at an optimal cost. In Texas, shifting towards value-based care has been a focus, with initiatives aimed at incentivizing healthcare providers to focus on patient outcomes and population health. Value-based care models promote preventive care, care coordination, and the integration of services across the healthcare continuum. These models aim to improve patient satisfaction, enhance health outcomes, and reduce healthcare costs. Embracing value-based care models, fostering collaboration between healthcare providers, payers, and patients, and promoting the use of evidence-based practices can contribute to a more efficient and effective healthcare system in Texas.
Telemedicine
Telemedicine, a subset of telehealth, involves the use of technology to provide clinical healthcare services remotely. Texas has seen a significant expansion of telemedicine services, with improved access to healthcare for individuals living in underserved areas or facing mobility challenges. Telemedicine allows for remote consultations, diagnosis, and even treatment delivery in some cases. It can improve access to care, reduce healthcare costs, and enhance continuity of care. Expanding telemedicine coverage, ensuring reimbursement parity with in-person visits, and addressing regulatory and licensure challenges are essential to fully leverage telemedicine’s potential and enhance healthcare delivery in Texas.
Community-Based Programs
Community-based programs play a crucial role in promoting health and preventing diseases. Texas has various community-based initiatives focused on specific populations or health issues. These programs engage community organizations, healthcare providers, and individuals to address health disparities, promote healthy behaviors, and enhance access to care. From chronic disease management programs to school-based health centers, community-based programs play a vital role in improving population health outcomes. Continued support for community-based programs, fostering collaboration between stakeholders, and addressing social determinants of health are essential to promote better health and well-being in communities across Texas.
In conclusion, Texas faces various challenges and opportunities in its healthcare system. Access to healthcare, quality of care, affordability, health outcomes, disparities, infrastructure, insurance market, healthcare policy, challenges, and innovations are central themes that shape the healthcare landscape in the state. Addressing these aspects requires a comprehensive and collaborative approach between healthcare providers, policymakers, community organizations, and individuals. By working together, Texas can strive toward a healthcare system that ensures equitable access, high-quality care, and improved health outcomes for all residents.